Transforming communities, families and individuals to flourish.
Featured Sponsor
Arizona’s Mental Health Crisis
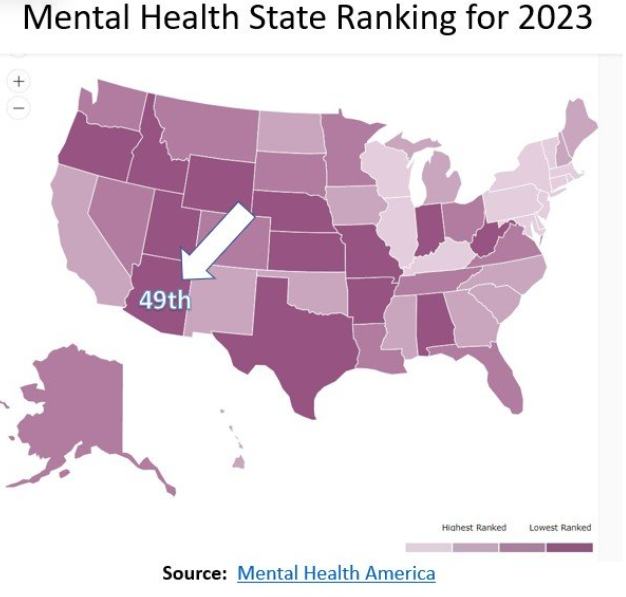
Arizona is facing a mental health and substance abuse crisis never seen before. What is shocking is the state ranks an appalling 49th as measured by the high rate of mental illness and low access to care, according to the 2023 State of Mental Health in America report. This is the moment for collective action and disruptive innovation to address this crisis across multiple fronts.
Read our Annual Report
The Healthy Communities and Wellness Alliance is a collaborative regional initiative to reimagine Arizona's behavioral health ecosystem. The Alliance partners with forward-looking organizations championing new healthcare models, next-generation workforce training, lifestyle change, and emerging technologies to improve health outcomes for communities, families, and individuals. The Alliance advances a whole-system problem-solving approach and helps partners design, prototype, and fund behavioral health solutions. The Alliance is an innovation accelerator enabling the health and wellness ecosystem to thrive.
All Hands On Deck!
Let's get to work!
Why Tucson should go big on AI healthcare
Conrad Plimpton and Egils Milbergs Special to the Arizona Daily Star
Nov 15, 2024
Tucson is at a crossroads of opportunity. With a burgeoning healthcare sector, robust research institutions, and a community eager for economic growth, Tucson can emerge as a leader in AI-driven healthcare.
Tucson’s research and healthcare strengths
Tucson’s significant advantage is its strong base in research and healthcare. The University of Arizona, known for its biomedical and information sciences programs, plays a central role. Banner Health — one of the region’s largest healthcare systems — provides fertile ground for research, clinical trials, and AI applications in healthcare. Tech Parks Arizona fosters academic, industry, and government collaboration, supporting AI research and development. The Center for Innovation is a leader in technology commercialization and is mainly involved in the biomedical field. Tucson has a solid foundation for piloting AI-driven tools in diagnostics, treatment planning, and administrative efficiency.
Building an AI-skilled workforce
Tucson should urgently prioritize workforce development in AI healthcare to realize this AI leadership opportunity. The need for a skilled AI workforce is pressing and crucial for the future of Tucson’s healthcare sector. Training local students, especially those from low-income or high-unemployment communities, in AI skills could help revolutionize patient care by addressing access, cost, and quality challenges.
Partnerships with organizations such as Pima Community College, Job Path, JTED, University of Arizona, Arizona State University, Pima County, and the City of Tucson should undertake a robust training initiative for AI, data science, diagnostics, patient monitoring, AI ethics, and digital privacy. This approach would close the regional healthcare skills gap, promote upward mobility, and reduce poverty. Wrap-around services, including transportation, childcare, food, and healthcare, would further support students from underrepresented neighborhoods to access better-paying careers.
AI’s role in addressing mental health
AI could help Tucson address mental illness and substance abuse in the region. Arizona faces a significant mental health crisis, ranking 49th nationally in terms of mental health prevalence and access. Southern Arizona suffers from a shortage of behavioral health professionals. AI could be a vital part of the solution.
AI tools like chatbots and virtual therapists offer immediate mental health support, reducing wait times and providing services in areas lacking mental health professionals. AI can analyze large health datasets to detect early signs of mental illness, suicidal tendencies, or substance abuse, allowing for early intervention. Additionally, AI can assist clinicians by analyzing patient data to support diagnoses and recommend treatment plans. AI-based training platforms can also accelerate the development of mental health professionals, filling workforce gaps in Tucson.
Economic benefits of an AI health ecosystem
The potential for AI applications in healthcare to reduce provider costs, improve patient outcomes, and streamline administrative processes is immense. AI healthcare is generative for business opportunities, tech startups, and investment.
A mentorship network connecting entrepreneurs with AI experts, healthcare providers, and essential resources could foster the growth of AI healthcare startups. These startups, in turn, would generate high-paying jobs, attract investment, and enhance Tucson’s standing in healthcare technology. Fostering AI health start-ups could help retain local talent. Too often, talented graduates leave Tucson for tech hubs like Silicon Valley or Austin. Strengthening the AI Entrepreneurial Ecosystem could reverse this brain drain.
Transforming healthcare access and outcomes
AI in healthcare can also significantly improve access and outcomes for Tucson’s underserved populations. Rural and low-income communities face barriers like limited transportation, a shortage of specialists, and long wait times. AI-driven tools, including telemedicine, predictive analytics, and automated diagnostics, could address these barriers by making healthcare more accessible and affordable. AI-enabled telemedicine can extend specialist care to remote areas, ensuring high-quality healthcare for all Tucson residents, regardless of location or income. This would not only enhance the health of Tucson’s population but also reduce healthcare disparities across the region.
Conclusion
The time for bold action is now. Tucson is uniquely positioned to lead in AI-driven healthcare. With solid research, healthcare, and innovation foundations, Tucson could become a national model for AI healthcare. AI healthcare can help drive Tucson’s economy, create high-paying jobs, attract investment, and improve regional health outcomes.
Check out this outstanding webinar:
Overcoming Arizona’s Behavioral Health Crisis: Roadmap to Wellness.
Aging Well Requires More Than Medicine: Why Whole‑Person Care Must Become the New Standard for Older Adults
Conrad Plimpton and Egils Milbergs
March 9, 2026
America is aging rapidly. Every day, more than 10,000 Americans turn 65, and most will live longer than any previous generation. Longevity should be a triumph of modern society. Instead, for many older adults, longer life has come with rising burdens of chronic disease, loneliness, depression, and fragmented care that too often responds late—after crises occur—rather than early, when prevention and support could make the most significant difference.
The problem is not that we lack medical expertise. It is that our healthcare system is not designed for the realities of aging. Older adults rarely experience illness in isolation. They live with multiple chronic conditions intertwined with behavioral health challenges, social isolation, mobility limitations, and loss of purpose. Yet care remains organized around brief office visits, single diagnoses, and siloed services, leaving patients and families to navigate complexity on their own.
If we are serious about improving outcomes and controlling costs in an aging society, we must rethink what health care for older adults actually means. The future of healthy aging will not be achieved solely through more procedures or medications. It will require a shift toward whole-person, preventive, and participatory models that address the complete set of factors shaping health in later life.
Chronic Disease Is a Lifestyle and Social Challenge
More than 90 percent of adults over age 65 live with at least one chronic condition, and most live with two or more. Heart disease, diabetes, arthritis, cancer survivorship, and cognitive impairment dominate clinical encounters. But the progression and impact of these conditions are powerfully influenced by nonmedical factors—physical activity, nutrition, sleep, stress, social connection, and daily routines.
Social isolation, in particular, has emerged as one of the most potent and underappreciated risks to older adult health. Loneliness is associated with higher rates of depression, dementia, cardiovascular disease, and premature mortality—at levels comparable to traditional clinical risk factors. The COVID‑19 pandemic made this painfully visible, as many older adults experienced abrupt disconnection from routines, services, and relationships that sustained their well-being.
Yet these drivers of health remain marginal to most care delivery models. Prevention accounts for only a small share of health spending, and social needs are often treated as peripheral rather than essential. The result is a system that excels at treating late-stage disease but struggles to help older adults maintain function, independence, and quality of life.
A Whole‑Person Alternative
Across the country, new models are beginning to demonstrate what a different approach could look like. Whole‑person aging models integrate medical care with lifestyle medicine, behavioral health, and social connection, recognizing that health is shaped as much by daily life as by clinical interventions.
One such approach is Holistic Aging 360, a community-anchored service designed to support older adults through personalized, predictive, preventive, and participatory care. Rather than waiting for decline, the model emphasizes continuous engagement by combining multidisciplinary care teams, telehealth, remote monitoring, lifestyle coaching, mental health support, and structured opportunities for social connection.
Participants receive individualized care plans aligned with what matters most to them, whether that is managing blood pressure, staying mobile, or remaining socially engaged. Data from regular check-ins and monitoring help identify risks early, while coaching and peer support empower individuals to take an active role in their health. Technology augments—not replaces- human relationships, allowing care teams to stay connected between visits and intervene before minor problems become major crises.
Importantly, whole‑person models treat social connection as a core health intervention, not an optional add-on. Group activities, peer support, volunteer engagement, and digital inclusion are built into the care model, directly addressing loneliness and isolation that undermine both mental and physical health.
Access Must Be Central
As interest in whole‑person aging models grows, healthcare access must be a central goal. . Older adults with lower incomes, limited digital access, disabilities, or from historically marginalized communities face greater barriers to care and worse outcomes. If new models rely solely on technology or private payment, they risk widening existing disparities.
Equitable aging models must therefore be designed for inclusion—offering hybrid in-person and virtual options, providing devices and digital literacy support, engaging caregivers, and adapting services to cultural and community contexts. Evaluation must examine who benefits and who does not, ensuring that improvements in outcomes are shared broadly.
Implications for Policy and Payment
The promise of whole-person aging models raises critical questions for policy and payment. While many of these services—care coordination, lifestyle coaching, social engagement—are not well reimbursed under traditional fee-for-service Medicare, they have the potential to reduce costly downstream utilization by preventing avoidable hospitalizations, emergency visits, and functional decline.
Medicare Advantage plans, accountable care organizations, and state aging agencies are beginning to explore how preventive, community-based supports can be aligned with value-based payment models. Philanthropy also has a critical role to play in de-risking innovation—supporting pilots, rigorous evaluation, and dissemination of lessons learned.
To scale what works, policymakers should consider how payment models can better support integrated, preventive services for older adults, including coverage for behavioral health, lifestyle interventions, and social supports that demonstrably improve outcomes.
A Call to Rethink Aging Care
Aging well is not solely a medical challenge—it is a societal one. As the population grows older, the question is not whether we can afford to invest in whole‑person aging models, but whether we can afford not to. Continuing to rely on fragmented, reactive systems will only deepen suffering and drive costs higher.
Whole‑person models offer a path forward—one that aligns care with how older adults actually live, honors dignity and purpose, and supports health long before crisis strikes. Making this approach the norm rather than the exception will require leadership from health systems, policymakers, payers, and philanthropy alike.
The future of healthy aging depends on our willingness to move beyond medicine alone and invest in the complete set of relationships and behaviors. It supports people in allowing them to thrive at every stage of life.
What is Behavioral Health?
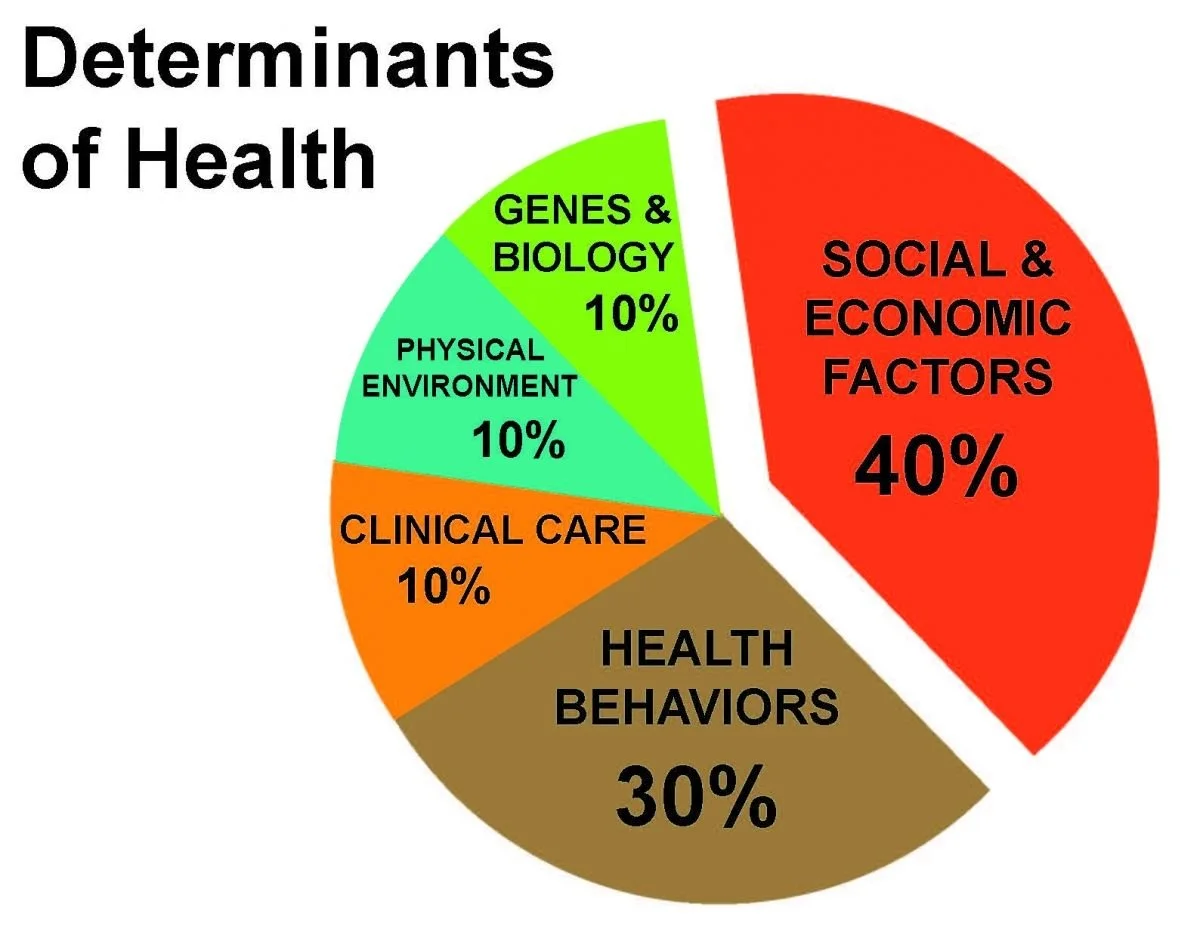
Behavioral health is the connection between a person's behaviors and overall well-being. It includes various conditions and disorders such as anxiety, depression, bipolar disorder, schizophrenia, suicidal thoughts, substance use disorders, and mental conditions impacted by social determinants of health (SdoH).
Behavioral health concerns how these conditions affect a person's daily life, relationships with others, and ability to function effectively. Behavioral health encompasses preventing, diagnosing, and treating these conditions and focuses on improving a person's overall quality of life.
Holistic Approach to Health
The COVID pandemic has demonstrated the need for an integrated and holistic approach to health and wellness rather than reactively providing treatments when sick.
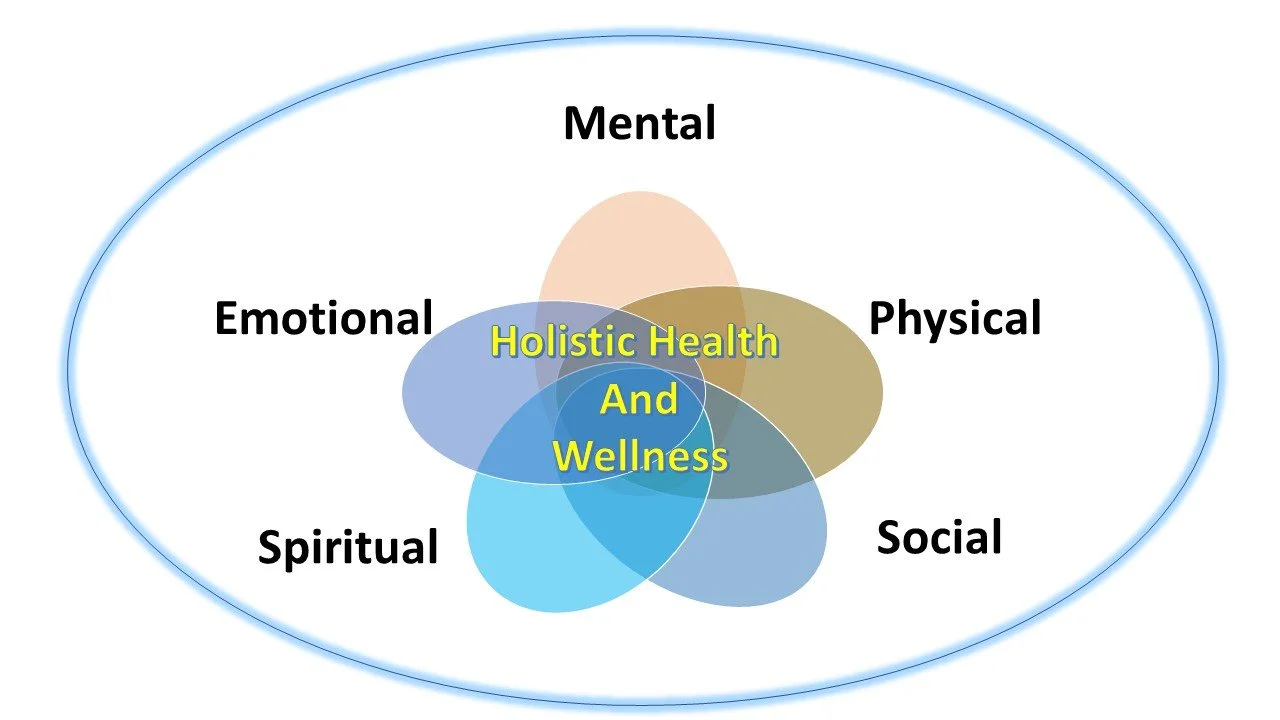
Holistic health and wellness refer to an approach that considers the whole person, including physical, mental, emotional, social and spiritual aspects. It is the idea that health is not just the absence of disease but the complete well-being of the body, mind, and soul. This approach emphasizes the importance of addressing all aspects of a person's life to promote optimal health, including nutrition, exercise, stress management, relationships, spirituality, and personal growth. Holistic health and wellness aim to create balance and harmony within a person to achieve overall health and happiness.
Healthcare is moving beyond siloed single-provider models to a cross-sector multi-layered care model. More healthcare providers are adopting holistic health concepts and becoming more proactive, preventive, participatory, technology-enabled, on-demand, and value-driven. Robust monitoring, communication, and artificial intelligence tools are augmenting diagnostics and treatments and developing options for home care and personal lifestyle skills.
Supporting Communities
Health and wellness happen within the context of a larger community. The Alliance works to ensure that our children, families, and individuals have the necessary tools, infrastructure, and spiritual support to flourish and live a healthy, longer, and purposeful life.